Can Face Masks Cause Yeast Infections?
Face masks have become a mainstay this year, thanks to COVID-19. You can find masks in an assortment of styles and colors as they have become a necessary fashion accessory to add to your wardrobe. But when the mask comes off, what is waiting underneath?
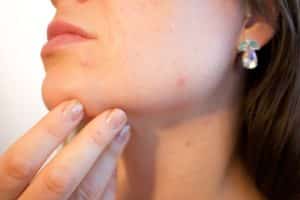
Some mask wearers are finding that the regular use of facial coverings are beginning to exacerbate skin conditions like acne and rosacea. Others are finding rashes on their faces they have never seen before. It turns out the warm, moist environment under the mask can be the ideal place for a yeast infection to develop.
Yeast Infections? On the Face?
Many women are all too familiar with yeast infections as they can be a common vaginal issue. However, most of us have never heard of a yeast infection affecting visible areas like the face.
It is the introduction of regular mask wearing that has brought this issue to light. Dr. Sapna Palep, founder of Spring Street Dermatology in New York City, recently broached the issue of yeast infections from mask wear. She has some basic facts about why they occur and what you can do to lower your risk.
Q: Is it possible to get a yeast infection on your face from wearing a mask?
Yes, absolutely! Dr. Palep warns that a yeast infection can occur anywhere there is warm, moist, creased skin.
Candida albicans is the most common culprit that takes advantage of this environment, which can be created by masks to create a superficial fungal infection.
Yeast is present on the skin and usually causes no ill effects. However, the right combination of factors can allow it to develop into an infection. It’s not the mask itself that causes the problem. But wearing a mask for extended periods of time, particularly in these hot, sticky days of summer, can encourage the factors that lead to infection.
Q: Does the summer heat play a role here in determining if a yeast infection will develop?
Dr. Palep explains that the area under the mask can generate heat and moisture, which creates an environment that is hospitable to a yeast infection.
Hot weather and humidity make it even easier for yeast to grow as these factors up the heat and moisture that builds underneath the mask. Pay special attention to those skin creases around the nose and mouth that are hidden under your mask.
While you may appreciate the ability to cover up those aging symptoms, they are also the places where yeast infections will thrive. If you notice any changes to the skin within those creases, contact your dermatologist.
Q: Are there certain skin types who are more predisposed to developing an infection like this?
Dr. Palep says that oilier skin types, such as acne, and this issue are more predisposed to a potential infection. On the flip side, drier skin types can also be susceptible to yeast infections.
In addition, people that suffer from other types of skin conditions are likely to see flare-ups with mask wearing that could raise their risk for infection. Conditions like eczema, in addition to rosacea and acne that Dr. Palep mentioned, can all become more problematic when under a mask for prolonged periods.
Q: Are there certain mask materials that are more predisposed to spreading this kind of infection?
Dr. Palep said the best thing you can do is look for a mask that uses a breathable fabric, like cotton. A lot of people can’t tolerate certain synthetic fabrics on their face.
Cotton is the best fabric for masks, as it’s the most comfortable and breathable on skin so you can wear it all day long. The worst materials to use are merino wool, cashmere, and lightweight ramie (like linen).
It is essential to wash your masks regularly, in a gentle detergent that is less likely to irritate the skin. Avoid soaps that have harsh chemicals or strong fragrances, as these are likely to set off a reaction that could make you more prone to bigger issues.
Q: Does the length of time in the mask make a difference in how likely you are to experience a reaction?
Most definitely. Dr. Palep explains that the longer you wear your mask, the more humidity, moisture, and sweat builds up, creating the perfect environment for yeast. In addition, the constant pressure of a mask causes cracks and fissures in the skin, which also produce an ideal environment for yeast.
Q: How do I know if I have a yeast infection?
Dr. Palep lists some of the warning signs as small raised blisters, pustules, rash, soreness, and chaffing. It’s important to see a board certified dermatologist immediately when you start to see the signs of it as it can worsen very quickly.
Q: How do I treat a yeast infection if I get one?
The good news is you can usually treat a yeast infection at home, using topical products. Dr. Palep recommends over-the-counter antifungal medications like miconazole, clotrimazole, or lotrimin. She warns that you should never use serums and oils on a yeast infection as they could worsen the condition.
Contact Spring Street Dermatology in Manhattan, New York Today
A yeast infection could be an unwanted byproduct of mask-wearing, but the good news is that if you catch it early, it can be treated easily with simple over-the-counter topical medications. If you are concerned about any changes to your skin as a result of your mask or are interested in medical or cosmetic dermatology treatments, contact our office today to schedule an appointment.
