Medical Dermatology in New York, NY
Spring Street Dermatology in New York is a comprehensive medical, surgical, and phototherapy treatment center. Our goal is to help each of our patients achieve healthy, beautiful skin through surveillance, individualized treatment and proper skin care.
Most Popular Medical Conditions
Skin Cancer
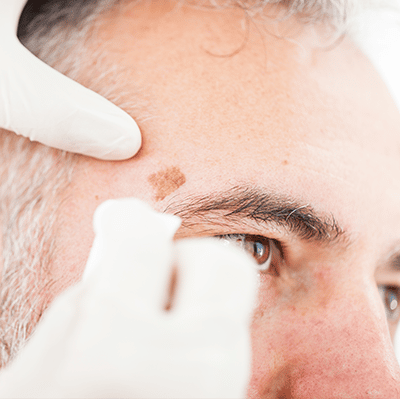
Melasma
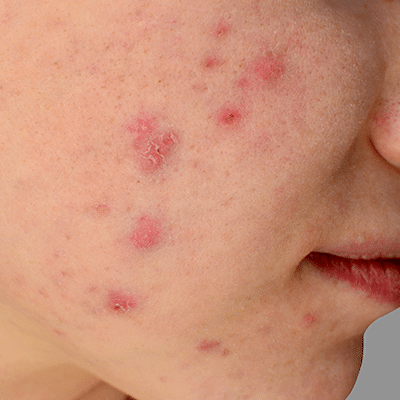
Acne
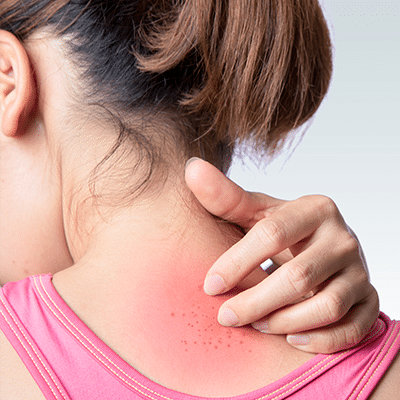
Eczema
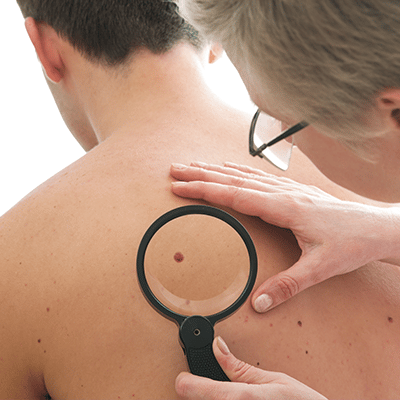
Brown Spots
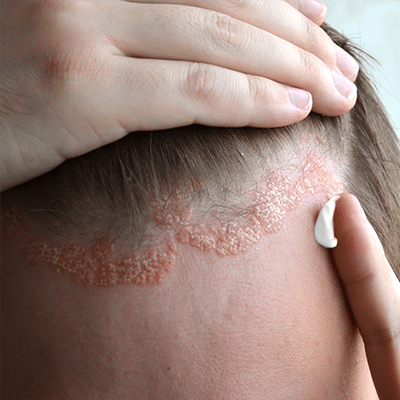
Psoriasis
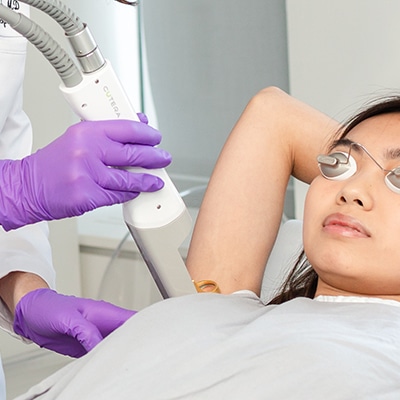
Hyperhidrosis
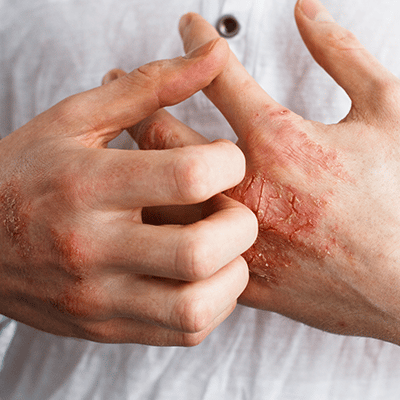
Hand Dermatitis
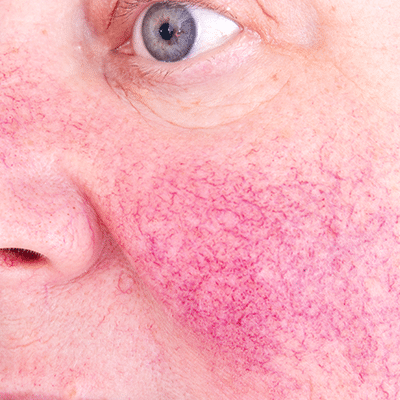
Rosacea
Sun Damage
All Medical Conditions
Acne
Acne is a skin condition with blackheads, whiteheads, red pimples and cysts. It usually affects the face, but can also involve the upper body. Acne affects people of all ages and in some, can leave dark marks or pitted scars.
Actinic Keratoses
Actinic Keratoses are precancerous skin lesions that may progress into squamous cell carcinomas. They usually occur in fair skinned individuals after years of sun exposure. Typical actinic keratoses are sandpaper-like rough, red spots that are more easily felt than seen.
Alopecia Areata
Alopecia Areata is a condition in which patients get small round patches of hair loss that usually grow back on their own, or may persist for years. It can happen to anyone, but is more common in people with a family history of the disease.
Atopic Dermatitis
Atopic Dermatitis is a type of eczema known as the “itch that rashes.” Between 10-20% of people in the world are affected and, in most cases, it begins to appear very early in life.
Bed Bugs
Bed Bugs (Cimex lectularius) are blood-sucking insects that infest old furniture, box springs, mattresses and bedding. They come out at night to feed on human blood. As a result, skin reactions to the bites are usually found in the mornings on skin not covered by sleepwear.
Benign Growths
A variety of non-cancerous, or benign growths, can appear in the skin over time. The cause of these growths is poorly understood, however, some are associated with aging and others run in families.
Contact Dermatitis
Contact dermatitis is a type of eczema that occurs when something that touches skin causes a rash. It can happen immediately or appear up to several weeks later.
Excimer
The excimer 308 nm wavelength light source is a targeted narrowband UVB (ultraviolet B) treatment option for localized eczema, psoriasis, and vitiligo. By targeting specific areas with an adjustable hand piece, light can be delivered to affected areas without exposing the whole body unnecessarily.
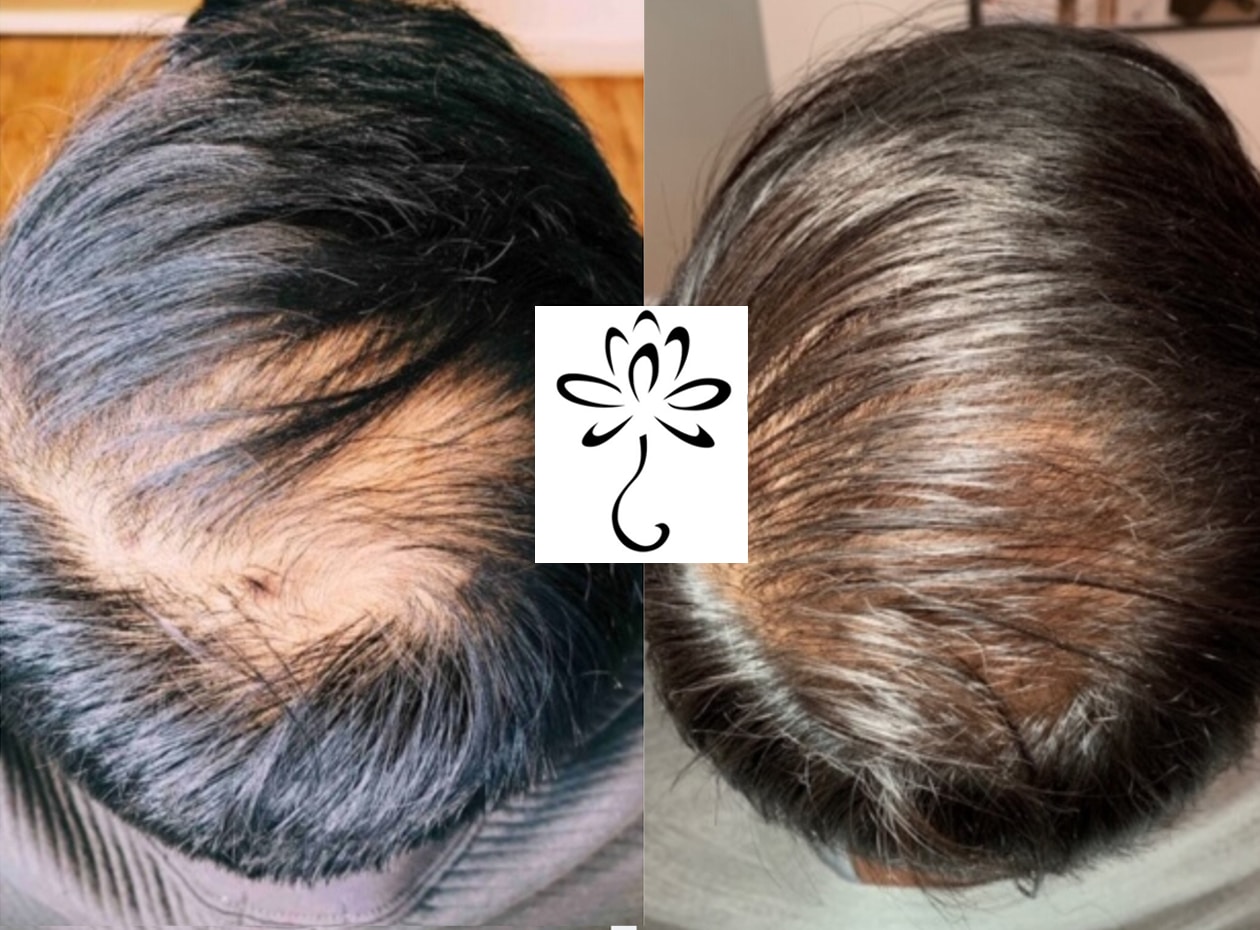
Hair Loss
There are various types of hair loss with differing causes. Some examples include androgenic alopecia, alopecia areata, telogen effluvium, and scarring alopecia.
Hand Dermatitis
Hand Dermatitis (also known as hand eczema) is characterized by hands that are dry, chapped, red, scaly and fissured. Sometimes, there may also be small blisters underneath the skin’s surface.
Herpes Simplex
There are 2 types of herpes simplex virus – I and II. Herpes Simplex Virus Type I usually causes cold sores, while Type II causes sexually transmitted genital ulcers.
Hirsutism
Hirsutism is the medical term for excess, male pattern hair growth in women. The cause may be high levels of circulating male hormone (testosterone) or increased sensitivity of hair follicles to the male hormone present.
Hyperhidrosis
Hyperhidrosis means excessive sweating. In most people, it occurs symmetrically on specific areas of the body, such as the underarms, hands, feet or head.
Lentigines
Lentigines are small light brown spots that occur in sun exposed areas, like the back of the hands or face, and tend to increase in number with age. They are harmless, but must be differentiated from moles and skin cancers.
Melasma
Melasma presents with brown patches on the cheeks, bridge of the nose, forehead and upper lip. It is most common in women of color and occurs more frequently in those with a family history of the condition.
COMING SOON: Mohs Surgery
Mohs surgery is a micrographic treatment for specific types of skin cancer, including basal cell carcinoma, squamous cell carcinoma, and some types of melanoma.
Molluscum
Molluscum contagiosum presents with skin colored bumps caused by a highly contagious virus. It is commonly encountered in school age children and, in adults, can also be spread by sexual contact.
Nail Fungus
Nail fungus is also known as onychomycosis. It affects about 12% of all Americans, can run in families and is more common in toenails than in fingernails.
Patch Testing
Patch testing is used for patients with dermatitis to find out whether substances coming into contact with the skin are causing or aggravating their condition. Potential causes of contact dermatitis include fragrances, preservatives, dyes, metals, plants and other chemicals.
Perioral Dermatitis
Perioral dermatitis is a form of rosacea that presents with redness, peeling and small red bumps in the area around the mouth, nose or eyes. Most often, young women are affected.
Photodynamic Therapy
Photodynamic therapy (PDT) is a procedure that uses a photosensitizing drug (Levulan Kerastick™ – aminolevulinic acid HCl) to apply light therapy selectively to target precancerous lesions, acne and sun damage. PDT can help clear actinic keratoses which are common premalignant lesions found in sun exposed areas.
Phototherapy
Phototherapy, or light therapy, involves exposing the skin to ultraviolet light on a consistent basis and under medical supervision. Present in natural sunlight, narrowband ultraviolet B (nbUVB) is a small range of ultraviolet light that effectively treats inflammatory skin diseases such as psoriasis, eczema, vitiligo, pruritus/ prurigo, polymorphous light eruption, mycosis fungoides and lichen planus.
Pityriasis Rosea
Pityriasis Rosea is a common rash that usually begins with a single, large scaly pink patch on the chest or back (the ‘herald patch’). Within a couple of weeks, additional lesions appear, often in a formation that looks like a Christmas tree over the back.
Psoriasis
Psoriasis is a chronic skin disorder characterized by raised lesions with silvery scale that most often occur on the scalp, elbows, knees and lower back. It can range from a very mild, hardly noticeable rash to a severe eruption that covers large areas of the body.
Rashes
All rashes may look similar – they can have blisters, blotches, and welts, and are usually red. While you may not correctly distinguish one rash from another, one thing is for sure: a rash can ruin a trip or a party for both kids and adults.
Ringworm
Ringworm is a very common fungal infection of the skin or hair. When ringworm occurs on the body, it is called tinea corporis. On the scalp, it is tinea capitis.
Rosacea
Rosacea is a common skin disease that causes redness and red pimple-like breakouts on the face. It begins with a tendency toward “flushing and blushing” and may then progress to a persistent redness of the central face.
Scabies
Scabies is an infestation of tiny mites that burrow under the skin. Within weeks, an allergic reaction with severe itching occurs. Itching is usually worst at night.
Seborrheic Dermatitis
Seborrheic dermatitis usually appears as a red, scaly, itchy rash on the scalp, in the eyebrows and on the sides of the nose. In infants, seborrheic dermatitis is called cradle cap.
Skin Cancer
Skin Cancer is the most common type of cancer in the United States. Light skinned individuals who burn easily are at greatest risk.
Sun Damage
Repeated and prolonged exposure to the sun results in sun damage. Skin damaged by the ultraviolet rays of the sun appears mottled, with uneven pigmentation and redness from dilated blood vessels.
Tinea Versicolor
Tinea versicolor looks like small, scaly, white, pink or brown spots and usually occurs on the upper arms, chest, back, neck or face. Because the fungus prevents the skin from tanning normally, the rash is usually most noticeable in the summer and on dark skin patients.
Vitiligo
Vitiligo is a skin disease which presents as symmetric white patches, most commonly on the face, lips, hands, arms, legs and genitals. Half of those affected are under the age of 20, and 1 in 5 have a family member with the condition.
Warts
Warts are noncancerous growths caused by an infection of the top layers of the skin by the human papilloma virus. There are several different types of wart and their appearance varies depending on their location.
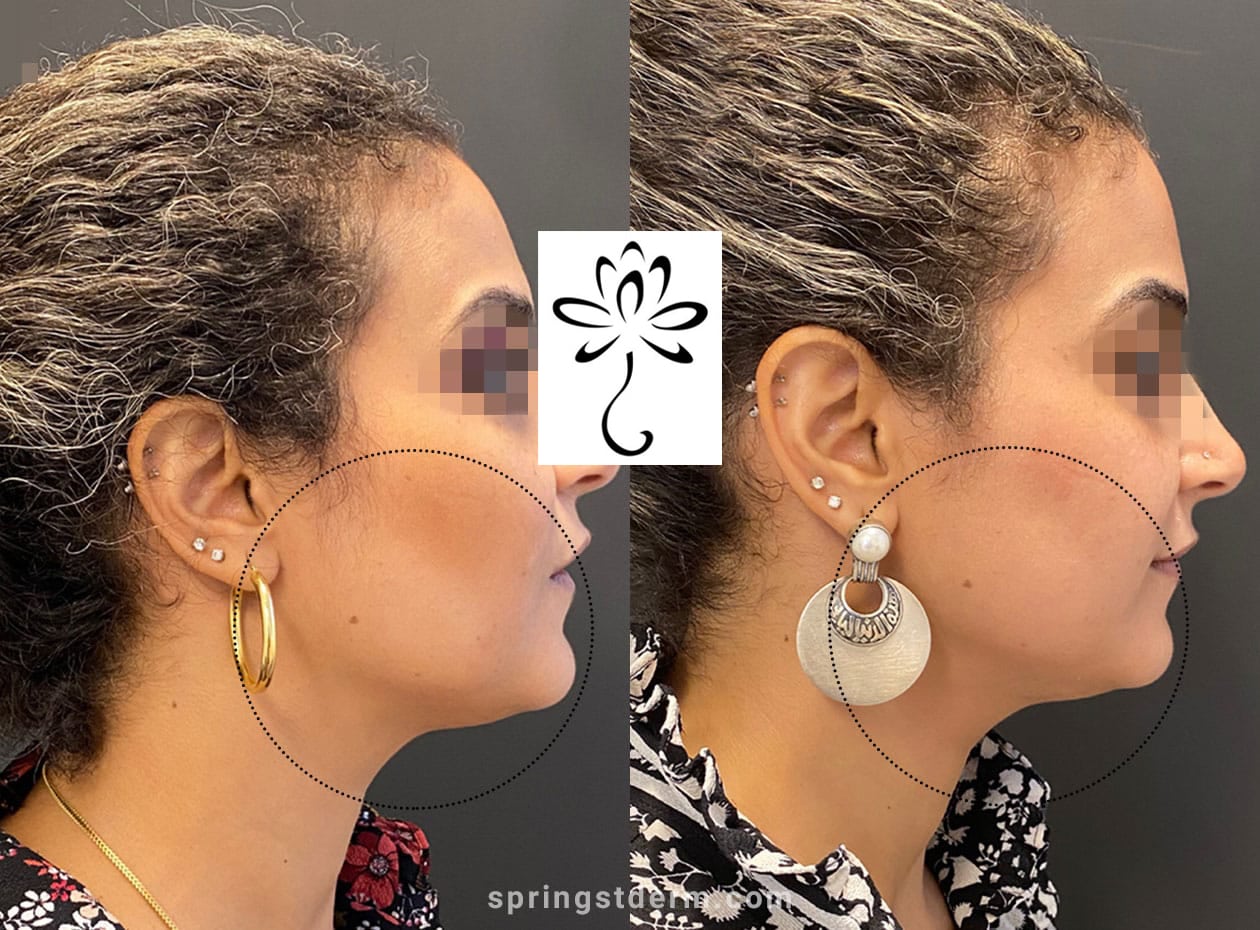
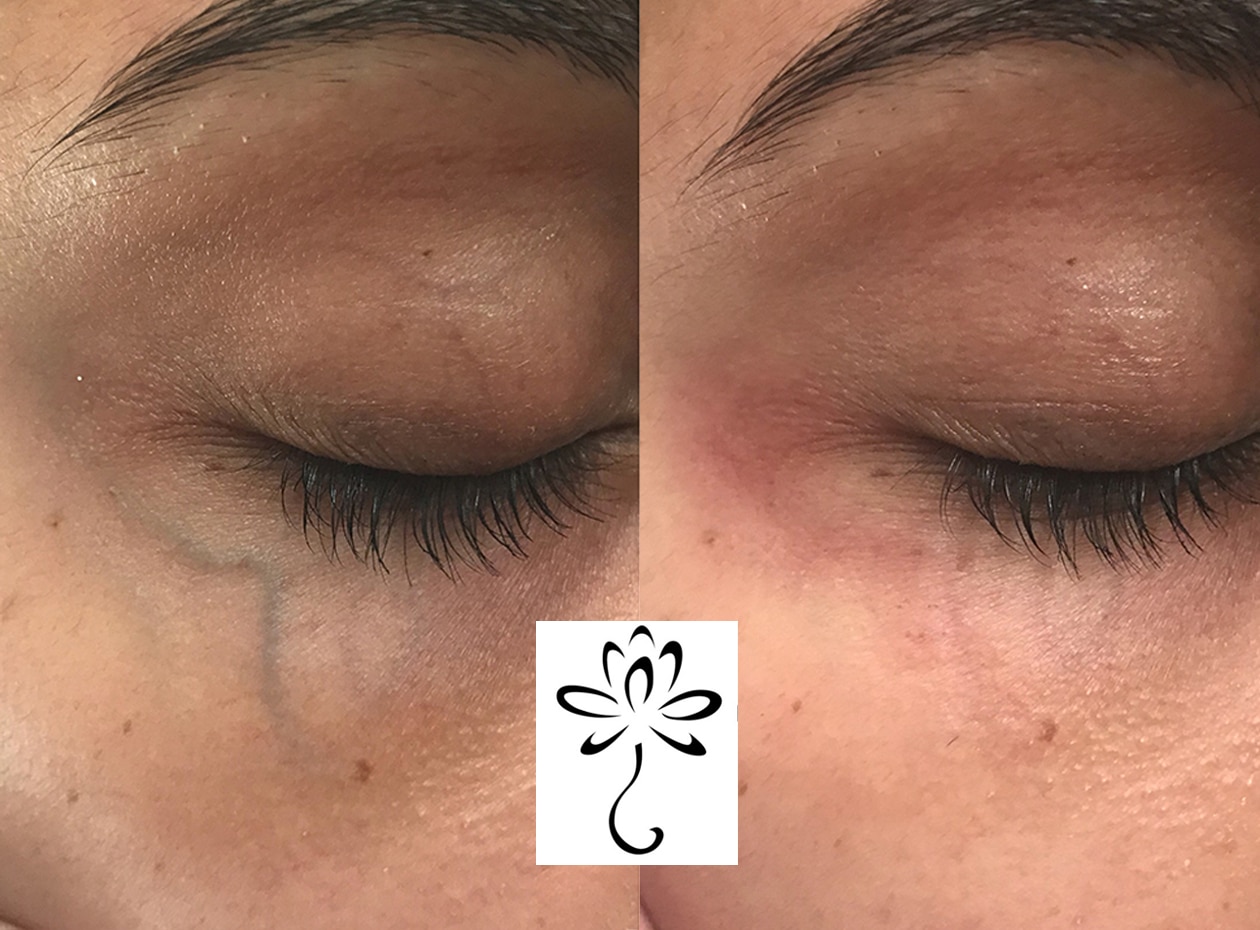
Before & After Photos
Thousands of New Yorkers Trust
Spring Street Dermatology
Contact Us
SOHO
75 Spring Street, Floor 2
New York, NY 10012
Monday - Friday: 8:00 am - 7:00 pm
Saturdays: 10:00 am - 4:00 pm
Same-Day Appointments Now Available
Uptown
4 West 58th Street, 13th Floor
New York, NY 10019
Monday - Friday: 8am – 6pm
Same-Day Appointments Now Available
| Title | Address | Description |
|---|---|---|
SOHO | 75 Spring Street, Floor 2 New York, NY 10012 | 75 Spring Street, Floor 2 |
UPTOWN | 4 West 58th street, 13th Floor New York, NY 10019 | 4 West 58th street, 13th Floor New York, NY 10019 Sun & Sat: 10am-3pm Mon-Fri: 8am-6pm |
Spring Street Dermatology | 75 Spring Street, Floor 2, NYC 10012 • 4 West 58th Street, Floor 13, NYC 10019 | 646.906.9614| Patient Portal | Pay Online
By Spring Street Dermatology now part of Schweiger | © 2026 All Rights Reserved. | Sitemap | Privacy Policy | The information available on this web site is provided for informational purposes only. This information is not intended to replace a medical consultation where a physician's judgment may advise you about specific disorders, conditions and or treatment options. We hope the information will be useful for you to become more educated about your health care decisions. If you are vision-impaired or have some other impairment covered by the Americans with Disabilities Act or a similar law, and you wish to discuss potential accommodations related to using this website, please contact us at 646.906.9614.